Chronic Wound Management: Strategies for Long-Term Healing
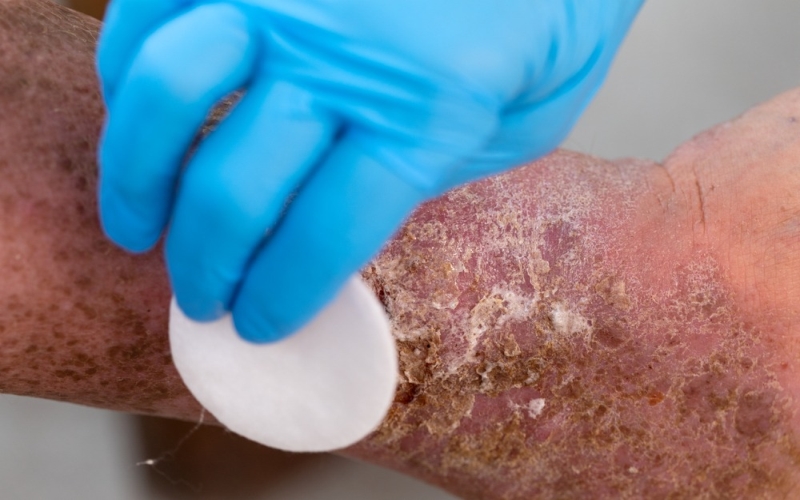
Living with a wound that just won’t get better is more than just a physical struggle. It can have a severe effect on your mental health, making every day a little tougher and every moment a nightmare.
Caring and healing from a chronic wound is no walk in the park. In this blog, we will talk about handling these kinds of wounds, focusing on improving them for the long haul.
We want to make sure you understand what chronic wounds are and why it’s important to manage them the right way.
Understanding Chronic Wounds
A chronic wound is one that hasn’t followed the natural healing process to restore both the structural and functional aspects within three months. It may have undergone repair without achieving a lasting and satisfactory outcome.
These wounds can be of different kinds, often called hard-to-heal or difficult-to-heal wounds or ulcers. It is commonly termed a chronic wound if a wound fails to heal between 4 weeks and three months. However, different healthcare professionals differ in the length of time associated with chronic wounds.
Importance of Effective Management of Chronic Wounds
Chronic wound care involves more than just putting a bandage on it and hoping for the best. It’s about figuring out the root cause of the problem and finding the best strategies to counter it.
Effective management of chronic wounds is crucial for several reasons.
- Prevents Risk of Complications: Chronic wound care and management help prevent complications like infections, lowering the risk of additional health issues.
- Improves Quality of Life: Secondly, it enhances the overall quality of life by managing the physical and emotional challenges associated with chronic wounds, promoting comfort and improved daily functioning.
Additionally, proper management tackles the emotional stress often linked to persistent wounds, alleviating anxiety and contributing to better mental health.
- Less Financial Stress: Minimizing the economic impact is another significant benefit, as well-managed chronic wounds can reduce the financial strain on individuals.
- Promotes Long-Term Healing: Moreover, tailored wound care and management strategies facilitate long-term well-being and improved quality of life.
Types of Chronic Wounds
Now that you have a basic understanding of chronic wounds let’s explore their different forms – each with its unique challenges and characteristics. Identifying the type of wound will help you determine the most effective strategies for healing.
In this section, we’ll take a closer look at some prevalent types of chronic wounds:
Pressure Ulcers:
These wounds develop from continuous pressure on a particular part of the body. Pressure ulcers are commonly found in individuals with limited mobility, such as those in wheelchairs or people who are bedridden. Proactive measures like position changes are the best way to prevent this chronic wound.
Diabetic Foot Ulcers:
As the name suggests, this chronic wound mainly occurs in the feet of diabetic patients. Diabetic ulcers, simply put, are stubborn wounds and need close monitoring by healthcare professionals for prevention and effective healing.
Venous Ulcers:
These chronic wounds develop from compromised blood circulation in the legs. Venous ulcers present a challenge in healing due to circulatory issues. The best way to counter this problem is to enhance blood flow to the damaged areas.
Arterial Ulcers:
Like venous ulcers, arterial ulcers are associated with inadequate blood flow through arteries and typically appear on the feet or toes.
Surgical Wounds:
Even impairments from surgical procedures can turn into chronic wounds without proper care. Proper post-op care and vigilant monitoring by healthcare professionals will prevent surgical wounds from transforming into chronic.
Understanding the distinct nature of each chronic wound will help create a tailored management approach for better outcomes.
The Impact of Chronic Wounds
Chronic wounds go beyond just medical concerns and affect all parts of a patient’s life. Therefore, patients, caregivers, and healthcare professionals need to understand the full impact of these wounds on an individual.
Here, we explore the three-fold effects of chronic wounds on a patient’s life, highlighting the importance of effective wound care strategies.
How Chronic Wounds Affect Physical Health?
Chronic wounds often lead to severe complications if not managed correctly.
Infection, one of the most severe complications, can lead to prolonged hospital stays, the need for surgical intervention, and, in severe cases, amputation or life-threatening systemic infections. Chronic wounds can also restrict mobility, leading to muscle atrophy and poor quality of life.
Emotional and Psychological Toll of Chronic Wounds
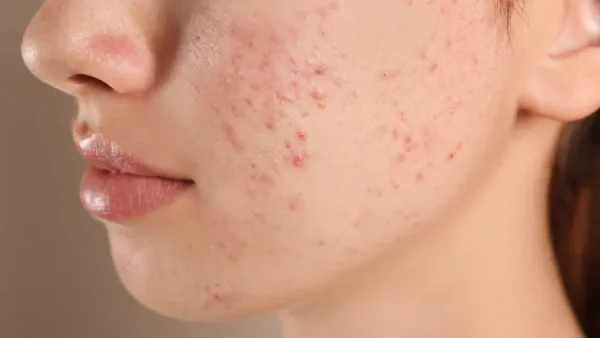
The impact of chronic wounds goes beyond physical symptoms, deeply affecting emotional and psychological well-being. Patients often experience depression, anxiety, and social isolation due to the persistent nature of their wounds and the limitations these impose on their daily lives.
The visibility of the wound can also lead to body image issues and a loss of self-esteem. This emotional stress affects the healing process, making psychological support an integral part of comprehensive wound care.
Economic Burden of Chronic Wound Care And Management
The cost of ongoing chronic wound care and treatment, including specialised dressings, medications, and advanced therapies like hyperbaric oxygen treatment, can be substantial.
For healthcare systems, chronic wounds consist of a significant portion of expenditure, often requiring long-term outpatient care and frequent hospital admissions. This impact extends to patients and their families, who may face financial strain due to medical bills and potential loss of income.
Understanding these economic challenges is crucial for healthcare administrators and policymakers to develop cost-effective strategies that do not compromise the quality of care.
Chronic Wound Assessment
A thorough and accurate examination of chronic wounds is the foundation of effective wound management. Here are the most critical components of chronic wound assessment:
The Importance of Clinical Evaluation in Chronic Wounds
Clinical evaluation is the first step in chronic wound assessment. Here are some of the indicators medical professionals look for:
- The Physical Attributes of the Wound: This evaluation includes a detailed examination of the wound’s size, depth, location, and the type of tissue involved, such as granulation, necrotic, or slough tissue.
- Wound Discharge: It also involves assessing the wound’s exudate or discharge – its amount, colour, and consistency. This is a vital indicator of the wound’s healing status.
- Skin Around the Wound: Besides the wound, clinicians assess the surrounding skin for signs of infection or other complications.
- Pain Level: Pain assessment is another critical aspect, as it can significantly affect the patient’s quality of life and wound healing.
This extensive clinical evaluation lays the groundwork for a tailored wound care plan to help the patients receive appropriate and effective treatment.
Utilising Imaging and Diagnostic Tests in Chronic Wound Care
Imaging and diagnostic tests offer a deeper understanding of the wound’s condition, helping in more accurate diagnosis and treatment planning. Here are some examples of how diagnostic imaging helps in chronic wound care:
- Ultrasound imaging looks into wound depth and the presence of foreign objects or underlying abscesses that are not visible to the naked eye during a physical examination.
- In cases of suspected bone involvement, like osteomyelitis in diabetic foot ulcers, X-rays, MRI, or CT scans can be vital.
- Wound cultures and biopsies are performed to detect infection or malignancy.
These diagnostic tools are essential for understanding the full extent of the wound and help healthcare professionals devise a more effective and targeted wound care strategy to promote quicker healing.
Key Principles of Chronic Wound Management
These fundamental principles ensure that treatment is thorough and tailored to individual patient needs. These principles guide health professionals, patients, and caregivers through the complex wound-healing process.
Here are five major principles widely followed in chronic wound care and management:
Wound Cleansing and Debridement
Wound cleansing involves removing contaminants to reduce infection risk. Saline solutions or specialised wound cleansers are commonly used for cleaning the wound.
Debridement – removing dead or infected tissue – is performed using surgical, mechanical, enzymatic, or autolytic methods, depending on the wound’s condition.
Effective cleansing and debridement prepare the wound bed for healing, allowing for better assessment and treatment planning.
Infection Control
An infected wound can delay healing, leading to systemic infections. Healthcare professionals use various strategies to control and prevent infection, including topical antiseptics, antibiotics, and advanced dressings with antimicrobial properties.
Regular monitoring is essential to ensure the wound is healing without interruption.
Moist Wound Healing
This approach reduces the risk of tissue dehydration and cell death and promotes new tissue growth around the damaged area. It also reduces pain during dressing changes.
Various dressings, such as hydrogels, alginates, and hydrocolloids, help maintain a moist environment while protecting the wound from external contaminants. Moist wound healing improves the patient’s comfort and the overall healing process.
Nutritional Support
A diet rich in proteins, vitamins, especially vitamins C and A, and minerals like zinc is crucial for repairing tissue and supporting immune function.
Patients with chronic wounds may have increased nutritional needs or may be at risk of malnutrition, which can inhibit the healing process.
Healthcare providers should assess the nutritional status of patients with chronic wounds and provide dietary recommendations or supplements as necessary.
Pain Management
Effective pain management strategies include wound dressings, pain medication, and techniques like cold therapy or relaxation exercises. Pain relief strategies comfort the patient and help heal wounds, as debilitating pain can hinder patient cooperation.
Personalised pain management plans, developed in consultation with the patient, are essential for a holistic approach to wound care.
Advanced Wound Care Technologies
Advanced technology has enhanced the quality of care for patients with chronic wounds. Let’s explore some of the cutting-edge methods currently transforming wound care:
Negative Pressure Wound Therapy (NPWT)
- Negative Pressure Wound Therapy (NPWT), or vacuum-assisted closure, involves creating a vacuum around the wound bed by applying controlled negative pressure.
- This helps to reduce edema, remove excess wound discharge, and promote perfusion and granulation tissue formation.
- NPWT is particularly effective for deep, large, or complex wounds and has been quite effective in treating diabetic foot ulcers and pressure sores.
Hyperbaric Oxygen Therapy (HBOT)
- In Hyperbaric Oxygen Therapy (HBOT), the patients breathes pure oxygen in a pressurised room or chamber, which increases the amount of oxygen in the blood.
- The increased oxygen supply in blood circulation helps to accelerate the natural healing process, especially in wounds where blood flow is compromised.
- HBOT has shown promising results in reducing swelling, fighting infection, and encouraging the growth of new blood vessels, making it a valuable tool in managing complex chronic wounds.
Growth Factors and Bioengineered Tissues
- Growth factors are proteins that stimulate cell multiplication and tissue repair. The topical application of these factors can speed up the natural healing of chronic wounds.
- On the other hand, bioengineered tissues are used to replace or support the function of damaged skin. These living, cell-based therapies can significantly enhance the healing process in wounds that have failed to respond to other treatments.
- These bioengineered products not only aid in closing wounds but also in restoring the function and appearance of the affected area.
Patient Education and Self-Care
Outcomes improve significantly when patients are well-informed and actively involved in their care.
Let’s explore how patient education and self-care can make a difference in managing chronic wounds.
Importance of Patient Involvement
Patient involvement includes understanding the causes of their wounds, recognising signs of infection or complications, and knowing when to seek medical attention.
Educated patients have been seen to follow through with care plans, attend follow-up appointments, and take proactive steps in their treatment.
Healthcare professionals can help patients become active participants in their healing journey, leading to better health outcomes and enhanced patient satisfaction.
Dressing Changes and Home Care Techniques for Chronic Wounds
This guidance ensures that patients or their caregivers can manage wound care effectively at home. Key aspects include:
- Instructions on how to clean the wound, apply new dressings, and identify signs of potential problems. For instance, patients or caregivers should know how to maintain a clean environment to minimise infection risk and understand the correct method of applying and removing dressings to avoid damaging new tissue.
- Additionally, it is important to educate patients to maintain a moist wound environment and dress the injury in the right manner.
Entrusting patients with these skills makes them confident and ensures continuity of wound care outside the clinical setting.
Surgical Interventions
Surgical procedures are considered when conventional treatments do not promote natural healing. Understanding these options is crucial for patients facing advanced stages of chronic wound care.
Here are some viable surgical options that are commonly used for chronic wounds:
Skin Grafts:
Skin grafting takes skin from one area of the body (the donor site) and transplants it to the wound site. This technique is often used for burns, extensive wounds, or wounds that expose underlying structures like bones or tendons.
Flap Surgery:
Flap surgery transfers a living piece of tissue with blood vessels that keep it alive, from one part of the body to another. This method is beneficial for covering deep wounds and providing skin, muscle, fat, and sometimes bone to the damaged area.
Amputation as a Last Resort
Amputation is the surgical removal of the affected limb or part of a limb and is considered the last resort in chronic wound management. It is considered when a wound, such as a severely infected diabetic foot ulcer, poses a risk to the patient’s life or when the limb cannot be saved.
The decision to amputate is complex and involves careful consideration of various factors, including:
- The patient’s overall health,
- The likelihood of wound healing and
- The impact on the patient’s life.
Patients and their families must thoroughly discuss amputation’s benefits, risks, and implications with their healthcare team.
Support systems, including counselling and rehabilitation services, help patients adjust to life after amputation.
Amputation is a difficult and emotional decision. However, it can sometimes be the best option for relieving the suffering and improving the overall quality of life in cases of severe chronic wounds.
Support and Resources
Managing chronic wounds extends beyond medical treatment; it encompasses a range of support and resources crucial for patients and their caregivers. This support not only aids in the physical aspect of healing but also addresses the emotional, psychological, and financial challenges of long-term wound management.
The Importance of Support Groups and Counseling
The journey of healing from a chronic wound can be a long and emotionally taxing one. Support groups and counselling are vital in providing emotional and psychological support.
Support Groups:
- Patients and caregivers get a platform to share their experiences, challenges, and coping strategies in these groups.
- It provides a sense of belonging and helps in reducing feelings of isolation and depression that often accompany chronic health issues.
Counselling:
- Professional counseling services help patients and caregivers manage chronic wound management’s emotional and psychological impacts.
- Counsellors offer strategies to cope with stress, anxiety, and the lifestyle changes that come with managing a chronic wound.
Exploring Financial Assistance Programs for Wound Care
Chronic wound care and management are burning a hole in your pocket, making exploring available financial assistance programs essential:
- Health Insurance Coverage: Many insurance plans cover a range of wound care treatments, but it’s essential to know the specifics, including any limitations or requirements for certain therapies.
- Charitable Organisations and Foundations: Numerous non-profit organisations and foundations offer financial assistance, resources, and educational materials to help manage the costs associated with wound care.
- Hospital and Clinic Programs: Some hospitals and clinics have programs or social workers who can assist patients in navigating financial challenges. They may offer sliding-scale fees or payment plans to make treatments more affordable.
Final Words
The journey to long-term healing of chronic wound management is both a physical and emotional one.
To everyone facing the challenges of chronic wounds, know you are not alone. Advances in medical science, coupled with comprehensive care strategies, are continuously improving the prospects of healing.
However, healing goes beyond technology and depends on the strength of human connection – through support groups, counselling, and the unwavering dedication of caregivers.
With resilience, support, and the proper care, long-term healing is not just a possibility; it’s within reach.